What is hidradenitis suppurativa?
Posted July 21, 2015 in Body Procedures by Josef Hadeed, MD
Hidradenitis suppurativa, also known as acne inversa, is a chronic inflammatory disease affecting the sweat glands. It is estimated to affect between 1-4% of the population. It commonly occurs in the creases or folds of the skin and is characterized by chronically recurring painful nodules that may form abscesses. The infection underneath the skin in turn leads to the discharge of pus. Drainage from the skin may result in constant soilage of the clothes, which can be a source of embarrassment. The underlying inflammation leads to scar formation and distortion of the skin. If left unchecked, this repetitive cycle of inflammation and infection can cause tunnels under the skin, resulting in sinus tracts that connect the various affected areas. The overlying skin ultimately becomes thickened.
What causes it?
The cause of hidradenitis suppurativa is unknown, although there are many suggested factors, including:
- Hormone imbalance
- Abnormal inflammatory response to skin follicle injury
- Reaction to chemicals found in deodorants and/or skin care products
- Heat and/or humidity
- Diet
- Hereditary factors
One of the prevailing theories into the genesis of hidradenitis suppurativa is that it starts with the production of hormones, which travel through the bloodstream to reach the follicles and sweat glands. Receptors within the follicles stimulate the production of cells that line the inside of the follicle, while the sweat glands produce more lubricant for the skin surface. The lining cells fail to separate from each other, forming an obstruction that prevents their normal transit to the surface of the skin. The continued production of lining cells and sweat results in a gradual expansion of the follicle, which eventually ruptures. The ruptured materials, which consist of several types of cells as well as bacteria, interact in the deep layer of the skin, leading to severe inflammation and the formation of nodules. The skin attempts to heal the follicle, but if it is unable to do so the inflammation spreads under the skin, leading to the formation of tunnels and additional scar tissue. There are several follicle-related diseases that are known to occur more frequently in patients with hidradenitis suppurative: acne, folliculitis decalvans (boils in the scalp), and pilonidal cyst (a boil-like process just above the tailbone).
How does hidradenitis suppurativa present?
Hidradenitis suppurativa is much more common in women than men (3:1 ratio). The majority of hidradenitis suppurativa patients have an elevated body mass index. Of note, approximately 30% of patients will have a history of other family members with hidradenitis suppurativa. There is a concentration of the disease to occur in folds of the skin, such 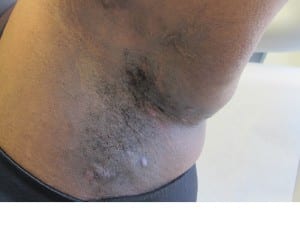 as the underarms, groin, buttocks, and in women under the breasts. Individual lesions may consist of small bumps occurring in these areas. These lesions may progress to become larger nodules or masses that look similar to boils. With repeated inflammation and scarring, sinus tracts develop under the skin. The lesions are typically painful and may drain foul-smelling pus. This cycle of repeated inflammation can persist for months or years. Hidradenitis suppurativa is one of the most unpleasant of all skin diseases. It causes pain, debility, embarrassment and self-consciousness. Its negative impact on patient quality of life is more than many other skin diseases.
as the underarms, groin, buttocks, and in women under the breasts. Individual lesions may consist of small bumps occurring in these areas. These lesions may progress to become larger nodules or masses that look similar to boils. With repeated inflammation and scarring, sinus tracts develop under the skin. The lesions are typically painful and may drain foul-smelling pus. This cycle of repeated inflammation can persist for months or years. Hidradenitis suppurativa is one of the most unpleasant of all skin diseases. It causes pain, debility, embarrassment and self-consciousness. Its negative impact on patient quality of life is more than many other skin diseases.
How is it treated?
There are both medical and surgical treatments for hidradenitis suppurativa. Because the cause of hidradenitis suppurativa is multifactorial, there is no single treatment that will be effective for everyone. There is currently no medication available to treat hidradenitis suppurativa. Medical treatment focuses on attempting to control inflammation within and surrounding the follicle. Various antibiotics have been used with different effectiveness. Dietary adjustment, weight loss, and smoking cessation may improve inflammation and reduce the trauma that leads to the rupture of follicles. Therapies directed at correcting abnormal hormone levels or blocking hormone receptors has been used with varied success. Retinoids, which can influence the growth pattern on the cells lining the follicles, have produced inconsistent results.
The preferred treatment for hidradenitis suppurativa is complete excision of the affected areas. Surgical treatment is usually offered to patients with more widespread disease not controlled with medical therapy. Surgical options range from excision of individual follicles, to wide excision of the affected area. If the entire area is excised, the resulting wound can either be left to heal in on its own, closed primarily, closed with a skin graft, or closed using local tissue flaps. Management of hidradenitis suppurativa must be individualized for each patient. It may be helpful to have a plastic surgeon surgically treat hidradenitis suppurativa to ensure optimal cosmetic outcomes. Surgery can provide extreme physical and psychological benefits for those suffering from this chronic, debilitating disease.
